
Baby tongue-tie division by fully trained and experienced practitioner
Gill Bird. Serving Hertfordshire, South Cambridgeshire and nearby areas
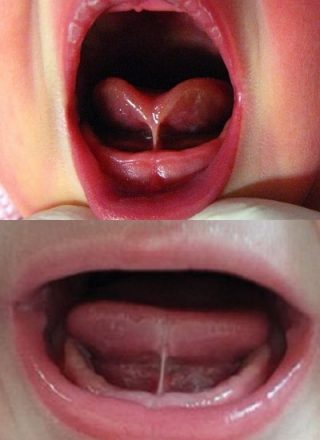
What's a Tongue-Tie?
It’s a very short or tight frenulum forming a tight string under the tongue. The tongue-tie can tether the tongue to the floor of the mouth and limit its free movement. This can often contribute to feeding problems, particularly with breast feeding. Moreover, it can also cause problems with weaning and later, oral hygiene. Some tongue-tied infants will not have any feeding problems apparent and so may not require treatment.
Tongue-tie division (Frenulotomy) is a quick, simple and safe procedure when performed on babies less than six months old. It involves swaddling the baby in a blanket, holding the baby still and cutting/releasing the tongue-tie. The baby needs to feed from the breast or bottle straight afterwards, as this stops any bleeding and comforts baby.
It’s therefore important your baby has not fed for one hour before my visit. There may be rare instances when, using clinical judgement, I decline to carry out the procedure.

My full name’s Gillian Bird, but I prefer Gill. I’m an experienced qualified midwife, trained in tongue-tie division at University Hospital Southampton. I carry out tongue-tie assessment and division in a private capacity in your own home and have insurance cover, CQC registration, ICO registration and NMC registration to permit me to do this work. I’m also a full member of the Association of Tongue-tie Practitioners and attend clinical updates. I do a high number of tongue-tie assessments and divisions, including at an NHS hospital.
I only see and treat infants under six months old.
How much does it cost?
You can make payment by cash, credit/debit card, contactless Apple Pay or Google Pay at the end of my visit.
I’ll send you a consent form for you just to read before my visit. It does not need signing before then. If a tongue-tie is found on examination and you decide to go ahead with the procedure the consent form is signed at that point by a parent or legal guardian.
A completed consent form and examination form is retained for my own records, but you may request a copy.
Immediately after a tongue-tie division, the baby needs to be put to the breast or bottle which settles bleeding and gives comfort. That’s why it’s so important that the baby is not fed for one hour before my visit.
The area under the tongue will be viewed after a feed and an aftercare leaflet and sticker given for baby’s red book.
I’ll call you seven days after my visit to check how your baby is getting on.
Tongue-Tie Division (Frenulotomy)
This includes a full assessment and the tongue-tie division procedure itself, where appropriate.
- Visits less than 20 miles travel £240
- Visits 20 miles and over £260
There may be an extra charge if the journey time is lengthy, involves tolls or charges, or has very limited parking availability.
Assessment Only
The full assessment includes a feeding and medical history, and physical examination to determine if a-tongue tie is present and its type.
- Visits less than 20 miles travel £140
- Visits 20 miles and over £160
FAQs
Will any local anaesthetic be used/does it hurt my baby?
No anaesthetic is used so the baby has maximum use of the tongue immediately afterwards to feed. The first feed settles bleeding. Fortunately, there are few nerve endings under the tongue, so it’s not thought to be very painful for the baby, maybe like a scratch. Babies generally seem to settle as soon as they feed. Babies over eight weeks of age may benefit from a dose of Calpol/liquid Paracetamol given one hour before my visit or later after the procedure.
What happens if my baby won’t feed straight after the tongue-tie procedure?
The wound can ooze blood for longer so a piece of gauze may need to be pressed on the wound. Much nicer to have a feed, which is why your baby should be hungry before the exam/procedure.
What is the chance of the Frenulum (tongue string) reforming after it has been cut?
There’s about 2-4% chance of this happening – it’s called re-attachment. Wound massage is popular in the US and at a few UK hospitals. However, it’s uncomfortable for baby, invasive to do, carries a risk of infection and isn’t backed up by research to have any positive effect. Simple tongue exercises will be taught.
What if anyone tests positive for COVID-19 soon after the home visit?
Please inform your tongue-tie practitioner so that consideration can be given whether to pause appointments. Likewise, your tongue-tie practitioner will alert you if she tests positive for Covid soon after your home visit. Please tell Gill if you have any Covid-like symptoms in your household up to the time of the visit.
What do parents say?
More than
Up to
Less than
Read the Complaint Policy here
Web design by Editorial & Creative Solutions LTD
